The Critical Care Medicine (CCM) Fellowship in the Department of Anesthesiology at WashU Medicine offers multidisciplinary training at one of the nation’s consistently ranking top-10 leading academic medical centers. The 12-month program is dedicated to preparing outstanding intensivists for rewarding careers in critical care medicine and provides comprehensive training in a supportive and stimulating environment.
Fellows spend at least nine months receiving clinical training in our various high acuity ICUs. The remaining three months are spent gaining focused expertise in a wide selection of electives. (We also offer an approved EM/CCM 24-month training cycle.) Fellows pursue mentored projects in basic or clinical research and receive weekly didactics from expert faculty. Critical care medicine fellowship applicants must be board-eligible in anesthesiology, surgery, obstetrics, or emergency medicine. The Accreditation Council for Graduate Medical Education (ACGME) has approved the program since its inception (over 25 years ago). The ACCM Fellowship has a close educational relationship with the Adult Cardiothoracic Anesthesiology Fellowship and annually recruits fellows into dual training slots for both programs.
The School of Medicine also offers critical care fellowship programs in surgery, pulmonary medicine, and neurology/neurosurgery. All CCM Fellowship programs work together to create a multidisciplinary training environment. The institution’s breadth of expertise in critical care medicine provides a rich learning environment for all its critical care fellows.
Trauma, burn, transplant, and surgical intensive care unit (SICU)
A closed ICU that comprises 36 beds allocated to an array of critically ill or injured surgical patients requiring pre-operative stabilization, post-operative intensive care after elective or emergency surgery, or critical care following complications of surgical illnesses. Patients admitted to the SICU arrive from all the surgical subspecialties, thus providing a broad base of experiences to trainees.
Cardiothoracic intensive care unit (CTICU)
A closed 36-bed unit devoted to the perioperative care of a diverse mix of routine and complex cardiac and thoracic surgical patients. Among other strengths, we have world-class lung transplantation, cardiac transplantation, mechanical cardiac support devices (LVAD, ECMO), complicated valvular repair/ replacement, and aortic repair programs.
Additional ICU’s
Fellows also spend mandatory time rotating in our academic medical ICU, dedicated surgical oncology ICU, and one of our large high acuity community mixed ICUs. Additional electives in the coronary care unit and neurology/neurosciences ICU are available. This broad clinical exposure ensures trainees will see the spectrum of critical care medicine pathology during their fellowship. Other intensive care units that play a significant role in our fellowship training include a dedicated oncology/BMT ICU, progressive care ventilator rehabilitation unit, and an emergency department trauma and critical care unit.
Our goal is to train fellows that are future leaders in the specialty of critical care medicine, and a multi-faceted didactic program underlies that goal. Our weekly multidisciplinary critical care lecture series (MDCCLS) provides the foundation for a strong base of knowledge. Attending faculty speakers from various disciplines participate, delivering a distillation of the most current thinking in all facets of critical care medicine. We also have a weekly Fellows Critical Care Lecture Series (FCCLS) with speakers from our own Division of Critical Care (view some of our previous recorded lectures). As part of the FCCLS, each fellow gives two lectures per year on the topics of their choice.
In order to ensure successful board certification post-graduation, we provide a robust CCM written board review lecture series. This also includes an in-service practice training exam during your fellowship year. Our goal is to provide trainees with all of the tools needed to become board-certified intensivists.
We have also developed a formal CCM ultrasound course aimed at preparing fellows for board certification in Advanced Critical Care Echocardiography now offered by the National Board of Echocardiography. Our CCM point of care ultrasound curriculum includes hands-on scanning, didactics, and case-based lecture review. We also have opportunities with transesophageal echocardiography (TEE) through a dedicated rotation, case-based lectures series, and simulation with our state-of-the-art TEE simulator.
At our monthly journal club and research-focused lectures, both faculty members and fellows participate in lively discussions inspired by the most current literature.
Our monthly clinical outcomes and unit-based quality Improvement meetings flush out the administrative component of training. These settings provide a forum to discuss patient safety and opportunities to improve our delivery of critical care medicine. Each fellow will be responsible for the completion of a quality improvement project which will often lead to publication opportunities.
Innovations in the education of our fellows are constantly being explored and expanded. Currently, we are collaborating with the nationally recognized Clinical Simulation Center at the WashU Medicine to develop novel approaches to fellowship, resident, and medical student education. We host hands-on procedural labs to round out exposure to all aspects of critical care (ventilator rounds, surgical airway lab, REBOA lab, etc). Additionally, we have a web-based critical care library (journal resources and taped lectures) that provide our fellows with a consistently up-to-date, accessible learning resource.
The Department of Anesthesiology is heavily funded by grants and consistently ranks among the top five nationally in NIH funding.
Clinical and basic science investigations occur in all the subspecialty areas, and many include partnerships with experts in other disciplines such as cardiology, hematology, or endocrinology. Fellows are offered mentorship in developing their own research projects, as well as encouraged to participate in ongoing research projects. All research seminars and research conferences are open to our fellows, and our monthly clinical research group is a valuable source of project development ideas.
We value national involvement, and all ACCM fellows receive membership in the Society of Critical Care Medicine (SCCM) and the Society of Critical Care Anesthesiologists (SOCCA). Fellows also have access to discretionary funds to facilitate attendance at national meetings.
This fellowship program participates in the San Francisco Match’s Central Application Service and is approved by the Accreditation Council for Graduate Medical Education (ACGME).
Critical care medicine trainees must be board-eligible in anesthesiology, surgery, obstetrics, or emergency medicine.

Brittney Gordon, MD
Emergency Medicine – Anesthesiology Critical Care Medicine Fellow (2026)
Residency: Emory University School of Medicine — Emergency Medicine
Medical School: George Washington University School of Medicine and Health Sciences

Adriana Grossman, MD
Dual CCM (2026)/ACTA (2027) Fellow
Medical School: University of Miami
Residency: University of Miami — Anesthesiology

Alexandra Hallagan, MD
Emergency Medicine – Anesthesiology Critical Care Fellow (2027)
Medical School: Ohio State University College of Medicine
Residency: Creighton University of Phoenix — Emergency Medicine

Raelyn Lorsen, MD
Emergency Medicine – Anesthesiology Critical Care Medicine Fellow (2026)
Medical School: University of Kansas School of Medicine
Residency: University of Utah — Emergency Medicine

Alex Lucas, MD
Emergency Medicine – Anesthesiology Critical Care Fellow (2027)
Medical School: Carle Illinois College of Medicine
Residency: Advocate Christ Medical Center — Emergency Medicine

Matthew Mannion, MD
Emergency Medicine – Anesthesiology Critical Care Fellow (2027)
Medical School: Southern Illinois University School of Medicine
Residency: Cleveland Clinic Akron General — Emergency Medicine

Joseph Miller, MD
Dual CCM (2026)/ACTA (2027) Fellow
Medical School: University of California, Riverside School of Medicine
Residency: WashU Medicine — Anesthesiology

Kaya Minezaki, MD
Emergency Medicine – Anesthesiology Critical Care Fellow (2027)
Medical School: Sackler School of Medicine, Tel Aviv University
Residency: Arrowhead Regional Medical Center — Emergency Medicine

Eleanor Montgomery, MD
Emergency Medicine – Anesthesiology Critical Care Fellow (2027)
Medical School: U Massachusetts Medical School – Worcester
Residency: University of New Mexico — Emergency Medicine

Nizar Osmani, MD
Emergency Medicine – Anesthesiology Critical Care Medicine Fellow (2026)
Medical School: University of Miami Miller School of Medicine
Residency: University of New Mexico — Emergency Medicine

Aunaly Palmer, MD
Emergency Medicine – Anesthesiology Critical Care Medicine Fellow (2026)
Medical School: University of Washington School of Medicine
Residency: Albert Einstein School of Medicine — Emergency Medicine

Melissa Pippin, MD
Anesthesiology Critical Care Medicine Fellow (2026)
Medical School: University of Mississippi School of Medicine
Residency: University of Mississippi Medical Center — Anesthesiology

Emilia Potter, DO
Emergency Medicine – Anesthesiology Critical Care Fellow (2027)
Medical School: Oklahoma State University College of Osteopathic Medicine
Residency: Oklahoma State University — Emergency Medicine

Ina Prevalska, MD
Emergency Medicine – Anesthesiology Critical Care Medicine Fellow (2026)
Medical School: The University of Texas Long School of Medicine at San Antonio
Residency: University of Michigan — Emergency Medicine

Peter Rafferty, MD
Dual CCM (2026)/ACTA (2027) Fellow
Medical School: Florida State University College of Medicine
Residency: UCF/HCA GME Consortium — Anesthesiology

Philip Smith, MD, PhD
Medical School: University of Maryland School of Medicine
Residency: WashU Medicine — Anesthesiology
Fellowship: WashU Medicine — Critical Care Medicine Fellow (2025-26)
* ASAP

Craig Sweeney, MD
Emergency Medicine – Anesthesiology Critical Care Medicine Fellow (2026)
Medical School: University of North Carolina School of Medicine
Residency: Virginia Commonwealth University Health System — Emergency Medicine
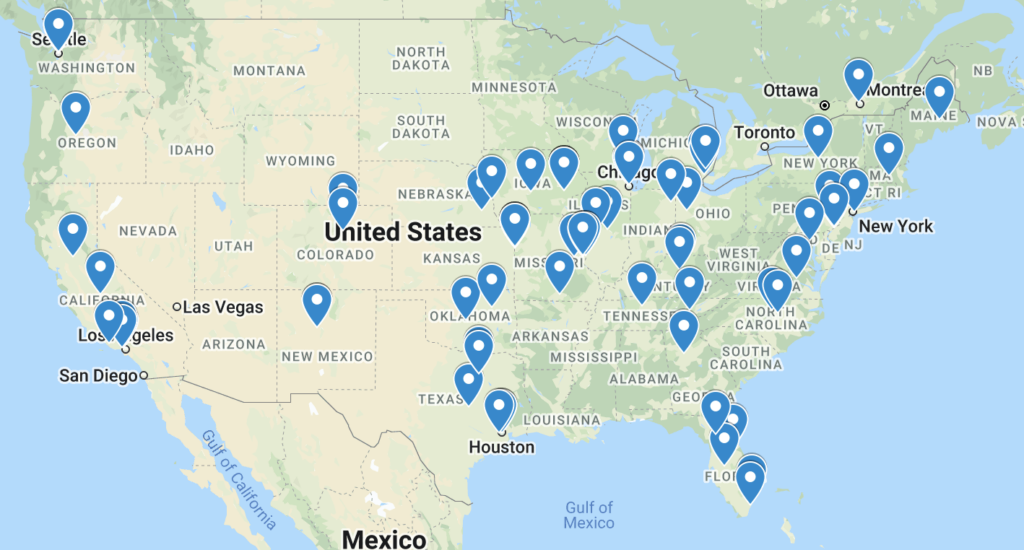
Where are our fellows now?
Our fellows go on to work at some of the top institutions in the world.
Data on the map below represents our past trainees from 1996.
