Our goal is to enhance the outcome of our patients undergoing surgery by helping patients avoid medical complications and promoting postoperative recovery.
At WashU Medicine, our patients receive perioperative care from international leaders in the field. We bring together compassionate clinicians, cutting edge technology, education and research to ensure every patient receives high-quality care. To achieve optimal health after surgical procedures, we believe:
- we must understand our patients. This includes their priorities, their medical problems, their skills, and their limitations.
- problems that may occur during and after surgery must be anticipated and prepared for.
- communication between patients and all of their clinicians must be promoted throughout their procedural journey.
- enhanced monitoring systems should be employed to detect changes in patient trajectories.
We are dedicated to promoting patient-centered and reliable health care from the moment surgery is scheduled to the day the patient returns to their normal life activities.
Patient Care

Preoperative Care
Patients planning to undergo a surgical procedure are evaluated by our medical staff at the Center for Preoperative Assessment and Planning (CPAP).
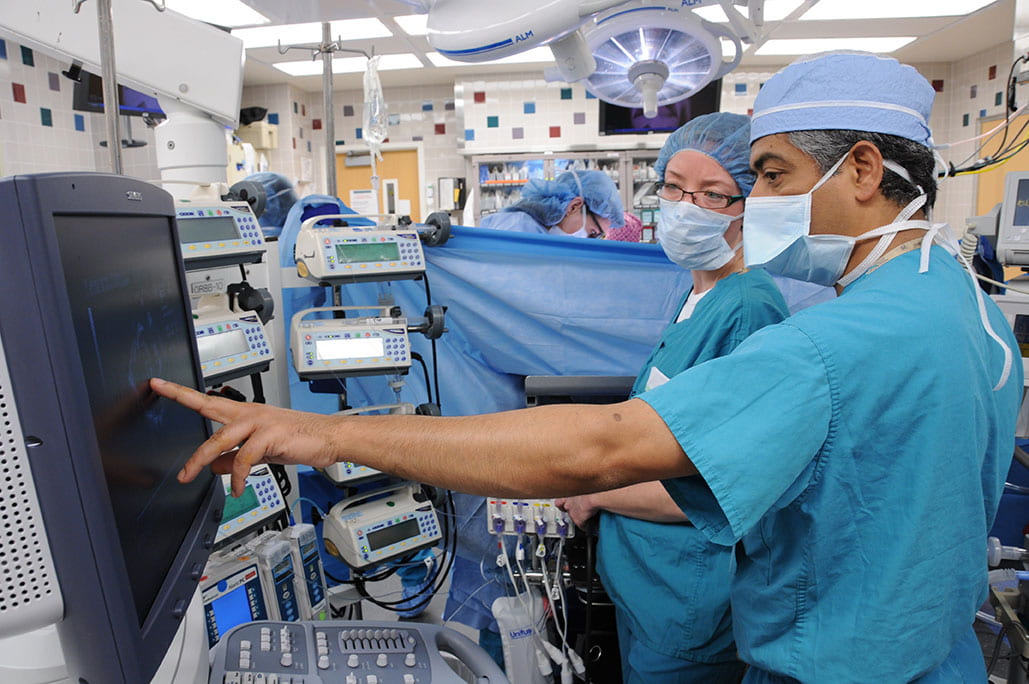
Intraoperative Care
On the day of their procedure, patients are cared for by anesthesiology clinicians specializing in a variety of areas of anesthesiology and surgery.

Post-operative Care
Our clinicians identify and prepare for each patient’s individual needs and possible complications. Our goal is to minimize complications after surgery and enhance our patient’s health.
Research
Our perioperative medicine team is persistently striving to improve patient care across the perioperative care continuum. The Department of Anesthesiology at WashU Medicine consistently ranks among the top five nationally in NIH funding and our division of perioperative medicine leads and participates in many studies spanning multiple divisions.
Our clinicians are continuously working to develop mechanisms to enhance the monitoring of patients during surgery and after surgery. Much of our research focuses on the development of systems to identify risk factors or problems that appear around the time of surgery. This allows clinicians to be able to more rapidly and reliably provide treatment for patients who may experience any problems.