The fellowship in Trauma Anesthesiology at WashU Medicine is one of only a few of its kind in the United States. The fellowship is a 12-month program and consists of OR rotations, ICU rotations, and elective rotations, as well as non-clinical time and time set aside for self-study, meetings/conferences, and educational activities. Seven months are devoted to OR anesthesia on the Trauma Anesthesia Service, focusing on preoperative clinical care, supervision of residents in anesthesiology, and administrative/triage management of the ORs. During this time, fellows will focus on caring for patients with acute traumatic injuries to the head, chest, abdomen/pelvis, spine, and extremities, urgent/emergent surgeries, as well as patients under Acute/Critical Care Surgery, Orthopedic Trauma, Vascular, ENT, and Neurosurgery. In addition, two months are spent as a Critical Care Fellow, managing critically ill patients in both the Neuro ICU and Surgical ICU. Electives compose the rest of the year and allow the fellow to learn a specialized skill or knowledge base from the trauma perspective. These rotations include Blood Bank/Transfusion Medicine, Critical Care Ultrasound/TEE, ER Radiology, Regional Anesthesiology, and Prehospital Management. Furthermore, fellows can choose to participate in global health projects offered by the Department of Anesthesiology if available. Fellows must obtain the ATLS certification at both the provider and instructor levels and are eligible to obtain basic echocardiography certification. Fellows also participate in departmental grand rounds, trauma service meetings, and conferences.
The fellow’s schedule is flexible, on average consisting of 16 shifts/month, which are served primarily alongside the Trauma Anesthesia attending. This time is split between supervision of CRNAs and residents or personally providing anesthesia for Acute Care Surgery, Orthopedic trauma, and neurosurgical patients while also being available for any urgent/emergent trauma cases that may occur throughout the day. In addition to clinical responsibilities, the trauma fellow assists with the administrative duties of OR staff management and triage, deciding what cases to start and hold based on OR workload and demand.
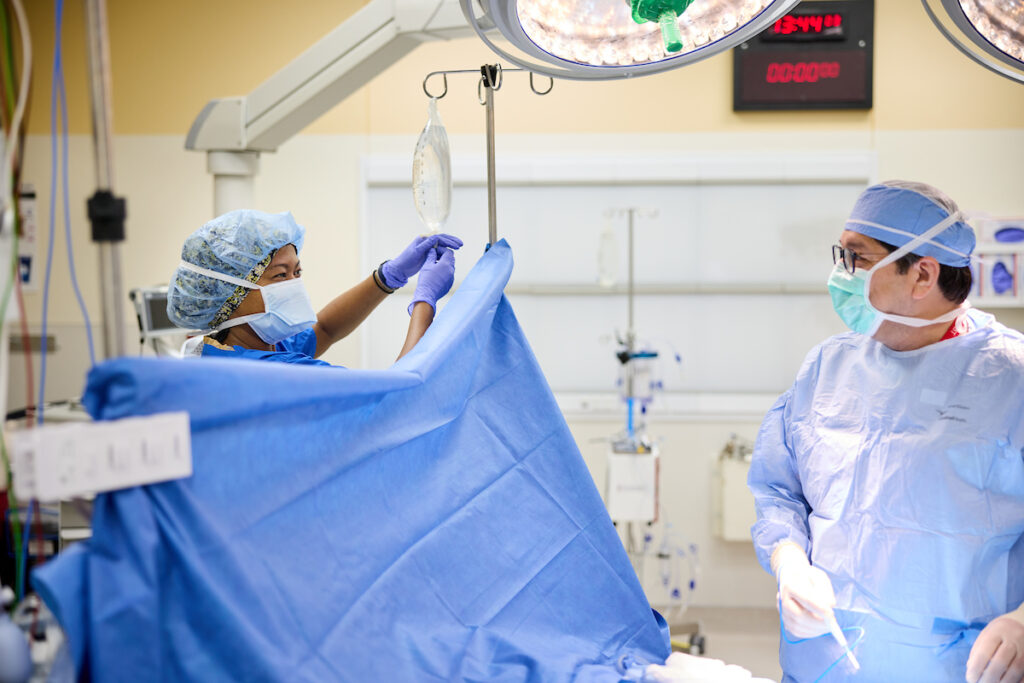
Fellows play an important role in the care of incoming trauma patients at the Emergency Department during their shift. They collaborate closely with a team comprising of Trauma Anesthesia attendings and colleagues from Trauma Surgery. During the initial assessment, trainees actively engage with Emergency Medicine and Surgery staff to contribute to the comprehensive evaluation and care of acute trauma patients. This involvement encompasses tasks such as airway management, line placement, resuscitation, imaging, and facilitating the patient’s transportation to the operating room.
Fellows actively engage in various educational conferences and activities related to Trauma Anesthesiology and the Department of Anesthesiology throughout the year. They assume an integral role in teaching residents during their Trauma Anesthesia rotations, which includes facilitating journal clubs, case conferences, and clinical teaching sessions. These educational activities take place in our simulation center and ORs. To support their professional development, fellows have one non-clinical day each week dedicated to work on projects and education. Additionally, they receive five meeting days to be utilized at their discretion throughout the year, allowing them to attend local, regional, national, or international conferences related to trauma care. Furthermore, fellows enjoy the benefit of 15 days of annual vacation time and receive a $1,500 discretionary fund from the department.
Current Fellows

Pegah Farhood, MD
Trauma Anesthesia Fellow (2025-26)
Medical School: Islamic Azad University
Residency: Tehran University of Medical Sciences — Anesthesiology & Critical Care Medicine
Alumni Fellows
| Name | Year |
|---|---|
| Julie Gillespie, MD | 2024-25 |
| Amrita Aranake-Chrisinger, MD | 2018-19 |
| Marcelino Murillo D’luquez | 2018 |
| Mahdi El Jallad | |
| Mary Hanna, MD, FRCPC | 2020-21 |
Fellowship Director

Jamie Brown-Shpiegel, MD
Assistant Residency Program Director of Recruitment, Integration, and Wellbeing; Program Director, Trauma Anesthesiology Fellowship; Assistant Professor, Anesthesiology; POD 4 Leader
- Email: jamiebrown@nospam.wustl.edu
Fellowship Coordinator
Interested in becoming a fellow?
- You should have completed an anesthesiology residency program, either in the United States or abroad, and passed the USMLE Steps for medical licensure.
- Please send your completed fellowship application and the following additional materials to Natasha Barclay:
- Personal statement
- CV
- Board certification(s)
- Headshot photo
- At least 3 letters of recommendation
- USMLE scores
- ECFMG certificate (IMG only)
- Visa eligibility (IMG only) – We accept a variety of visas but cannot sponsor new H-1 visa applications at this time. Our program is open to considering applicants who are currently on a H1B visa, but please note that we cannot guarantee sponsorship of any particular visa.
- Selected candidates will be interviewed via telephone or Zoom, followed by an optional in-person campus visit at the candidate’s request.
- Our fellowship program director, along with division leadership, will evaluate candidates based on residency performance, recommendations, and a demonstrated interest in trauma care.

